Anecdotally, there do seem to be more news reports of necrotizing fasciitis a serious, quickly spreading and potentially deadly bacterial infection sometimes dubbed “flesh-eating bacteria” in warmer months. Even though research is limited, some studies have confirmed this trend, including a 2019 paper published by the Saudi Medical Journal that found necrotizing fasciitis cases increased during hot and less humid weather in Nova Scotia, Canada. “Necrotizing fasciitis is thought to be more common in the summer because people are more likely to have exposed skin,” explains Anisha Patel, MD, a dermatologist at MD Anderson Cancer Center in Houston, Texas.
But before you panic, realize that your chances of developing it are very low. The incidence ranges from between 0.3 to 15 cases per 100,000 people—or between 0.0003 and 0.015 percent. And according to an estimate from the National Organization for Rare Disorders, necrotizing fasciitis is so uncommon that doctors on average see only two cases during their careers.
Still, the Centers for Disease Control and Prevention (CDC) says that 700 to 1200 cases are reported to it each year. Here’s what you need to know about this rare—but potentially devastating disease. Necrotizing fasciitis is most often caused by group A Streptococcus bacteria, says Dr. Patel. This is the same type of bacteria that causes strep throat. But according to the CDC, other bacteria such as Klebsiella, Clostridium, Escherichia coli (E. coli), Staphylococcus aureus and Aeromonas hydrophila, Bacteroides, Clostridium, Pseudomonas and Prevotella can also cause these infections. In warmer seawater, necrotizing fasciitis can also be caused by Vibrio vulnificus bacteria. where, including on our own skin. Most of the time they’re harmless, causing no symptoms or perhaps milder skin infections such as impetigo.
But sometimes, when your skin or mucus membranes are breached or otherwise compromised such as from a puncture wound, laceration, insect bite, blunt trauma injury, or surgery these bacteria can infiltrate your body, infecting your fascia, the connective tissue that surrounds your muscles and organs.
Many of these types of bacteria can be found in almost any “The classic case scenario is someone at the beach goes into the water with an open cut that allows bacteria to enter the skin,” explains Patel. As the infection rapidly spreads, the bacteria attack and destroy the surrounding tissue. If left untreated, toxins secreted by the bacteria may lead to septic shock or toxic shock syndrome. In the worst-case scenario, the infection may cause the loss of a limb or even death in 30 percent of cases. The good news is, if you’re young and healthy with a tip-top immune system, you’re extremely unlikely to pick up a case of necrotizing fasciitis, reassures Patel. Most of the time, people who come down with this disease have other health conditions that make it harder for their bodies to fight off infection. This includes people with type 2 diabetes, kidney disease, hepatitis B or C, HIV, and cirrhosis as well as people undergoing chemotherapy due to cancer or those on medications that suppress the immune system. “I’ve only seen two cases of necrotizing fasciitis in my entire career,” says Patel. “It was in two very ill people who were already severely immunocompromised.”
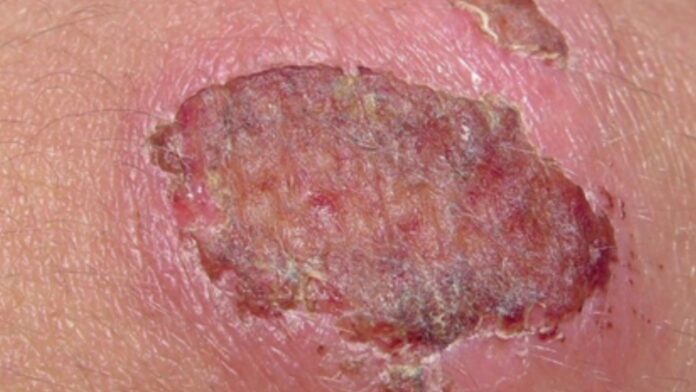
Symptoms to watch for Necrotizing fasciitis may begin uneventfully, with soreness resembling a pulled muscle. From there, the condition can progress rapidly, as the skin typically becomes red, swollen, and warm to the touch, with the onset of severe pain that may seem out of proportion to the apparent injury. Fluid- or gas- filled blisters may form as the skin darkens.